GERD is often linked to heartburn or indigestion, but it can also affect breathing. Some people experience chest tightness or difficulty taking a deep breath, which can be mistaken for heart or lung issues. Repeated acid reflux irritates the esophagus and nearby nerves, sometimes triggering coughing, throat discomfort, or shortness of breath.
While breathing issues are usually temporary, severe or persistent symptoms require prompt care. Searching for an emergency room near me can ensure quick evaluation and treatment for serious conditions that may resemble or worsen GERD-related respiratory problems.
What is GERD and Its Impact on the Body
GERD, or gastroesophageal reflux disease, is a chronic digestive condition in which stomach acid frequently flows back into the esophagus. Normally, the lower esophageal sphincter (LES) acts as a valve to prevent acid from moving upward, but when this valve weakens or relaxes at the wrong time, acid reflux occurs. While occasional reflux can happen to anyone after a large meal, GERD involves repeated and persistent episodes that can irritate the esophagus and surrounding areas, including the throat and airways.
Common symptoms of GERD include heartburn, regurgitation of food or sour liquid, chest discomfort, persistent cough, throat irritation, and a feeling of fullness or bloating after meals. Although many symptoms may remain mild, chronic reflux can lead to complications if left untreated, particularly when respiratory symptoms such as shortness of breath or wheezing begin to appear.
What Does GERD Feel Like?
The sensations associated with GERD can vary from person to person. The most common symptom is a burning sensation in the chest, often called heartburn, which usually occurs after eating or when lying down. Some people may also experience a sour taste in the mouth when stomach acid moves upward. Other common signs include frequent burping, nausea, throat irritation, or a persistent cough that is not related to a cold.
In some cases, GERD can create pressure or tightness in the chest, making breathing slightly uncomfortable. Because these symptoms can resemble heart or lung issues, they may cause anxiety. If discomfort is severe or persistent, contacting an emergency room Lake Jackson, TX can ensure prompt evaluation and rule out more serious conditions.
How Does GERD Cause Shortness of Breath?
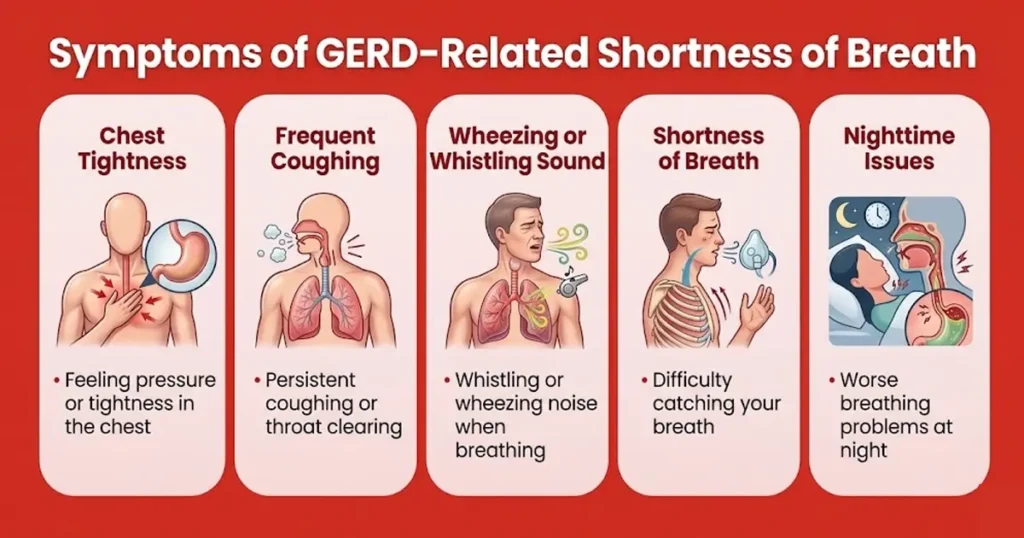
Although GERD primarily affects the digestive tract, it can influence breathing in several ways. The esophagus and the respiratory system are located in proximity to each other in the chest, and irritation from stomach acid can affect nearby structures.
Airway Irritation
When acid repeatedly reaches the upper part of the esophagus, it may irritate the throat and airway lining. This irritation can trigger coughing, throat clearing, or a sensation of restricted breathing. In some individuals, the airway becomes sensitive to acid exposure, which contributes to shortness of breath.
Acid Reaching the Airways
In certain situations, tiny amounts of stomach acid may travel into the upper airway. Even very small amounts can cause inflammation or irritation in the respiratory passages. This may lead to symptoms such as wheezing, coughing, or difficulty breathing deeply.
Triggering Bronchospasms
Acid reflux can stimulate nerves connected to the lungs, causing the airways to tighten temporarily. This tightening, known as bronchospasm, can cause asthma-like symptoms, including wheezing and shortness of breath.
Nighttime Reflux and Breathing Problems
Shortness of breath related to GERD often becomes more noticeable at night. Lying flat allows acid to move upward more easily, which can irritate the throat and airways during sleep. As a result, some people wake up coughing or feeling as though they cannot breathe comfortably.
These mechanisms explain why GERD is sometimes associated with respiratory symptoms, even though the condition typically begins in the digestive system.
How to Treat GERD-Related Shortness of Breath
Treating GERD-related breathing discomfort focuses on controlling acid reflux and reducing irritation in the esophagus and airways.
Lifestyle Changes
Many cases improve with simple lifestyle adjustments. Eating smaller meals, avoiding late-night eating, and remaining upright for a few hours after meals can help prevent acid reflux by preventing acid from moving upward. Elevating the head of the bed may also reduce nighttime reflux.
Maintaining a healthy weight and limiting trigger foods, such as spicy meals, caffeine, fatty foods, and carbonated drinks, can further reduce reflux symptoms.
Medications
Doctors often recommend medications that lower stomach acid levels. Antacids provide quick, short-term relief, while H2 blockers and proton pump inhibitors (PPIs) reduce acid production for longer periods. These medications help the esophagus heal and prevent irritation that could affect breathing.
Medical Evaluation
If symptoms persist or worsen, a healthcare provider may recommend diagnostic tests to confirm GERD and assess its impact on the esophagus and respiratory system. These tests may include procedures such as endoscopy, pH monitoring, or imaging studies to evaluate acid reflux and possible complications.
When GERD Is Dangerous
Although GERD is common, persistent reflux can lead to complications if not managed properly. Long-term acid exposure may cause inflammation of the esophagus, known as esophagitis, resulting in pain or difficulty swallowing. Repeated irritation can also lead to changes in the esophageal lining, called Barrett’s esophagus, which increases the risk of esophageal cancer over time.
GERD can affect the respiratory system, triggering chronic coughing, worsening asthma, or causing throat irritation. If symptoms are severe, sudden, or affect children, seeking an emergency room for pediatrics ensures immediate evaluation and proper care for potentially serious complications.
How to Prevent GERD
Preventing GERD symptoms often involves simple daily habits that reduce acid reflux and protect the esophagus.
- Eat moderate portions: Avoid overeating, as large meals increase stomach pressure and make reflux more likely.
- Avoid late-night meals: Try not to eat heavy meals close to bedtime, since lying down soon after eating can trigger acid reflux.
- Limit trigger foods: Reduce consumption of fried foods, chocolate, spicy meals, caffeine, and highly acidic foods that may increase acid production.
- Maintain a healthy weight: Excess body weight places additional pressure on the stomach, which can cause acid to reflux into the esophagus.
- Avoid smoking and excessive alcohol: Both can weaken the lower esophageal sphincter, making it easier for acid to flow back into the esophagus.
Following these habits consistently can help reduce reflux episodes and lower the risk of developing chronic GERD symptoms.
When to Go to the ER?
While GERD symptoms are often manageable, certain warning signs require immediate medical attention because they may indicate a more serious condition.
- Severe or sudden chest pain: Intense chest pain, especially when accompanied by shortness of breath, may indicate a heart-related issue and should be evaluated promptly.
- Shortness of breath with dizziness or fainting: Difficulty breathing, along with confusion, fainting, or severe dizziness, can signal a medical emergency that requires urgent care.
- Persistent vomiting: Ongoing vomiting can lead to dehydration and may indicate severe irritation or complications related to GERD.
- Severe coughing or wheezing: Continuous coughing, wheezing, or breathing difficulty that does not improve could indicate airway irritation or another respiratory issue.
- Difficulty swallowing: Trouble swallowing food or liquids may indicate inflammation or narrowing of the esophagus, which requires prompt medical attention.
In these situations, visiting the Altus Emergency Center allows healthcare professionals to quickly rule out heart or lung emergencies and provide appropriate treatment.
Key Takeaways
- GERD is a chronic digestive condition caused by frequent acid reflux.
- In some cases, GERD can lead to respiratory symptoms, including shortness of breath.
- Acid irritation, airway inflammation, and bronchospasms are common mechanisms linking GERD to breathing difficulties.
- Lifestyle changes, medications, and medical evaluation can help manage symptoms effectively.
- A healthcare professional should always assess persistent or severe symptoms.
FAQs
What foods are good for GERD?
Foods that are low in fat and non-acidic, such as oatmeal, bananas, melons, lean proteins, and vegetables, are generally gentle on the stomach and less likely to trigger reflux.
How to treat GERD naturally?
Natural approaches include eating smaller meals, avoiding trigger foods, maintaining a healthy weight, elevating the head during sleep, and practicing stress-reduction techniques.
How long does GERD last?
GERD is a chronic condition that can persist for months or years if not managed properly, though symptoms may improve with lifestyle changes and medication.
Summary
GERD is often recognized for causing heartburn, but its effects can extend beyond the digestive system. In some individuals, repeated acid reflux can irritate nearby nerves and airways, leading to coughing, chest tightness, or shortness of breath. Recognizing these symptoms early is crucial because untreated reflux can lead to complications. With appropriate lifestyle changes, medications, and medical guidance, most people can successfully control GERD symptoms and prevent breathing-related discomfort.

